|
Abstract Ganglions are the
most common soft tissue tumour of the hand1. Ganglion of the
proximal interphalangeal joint however, is rare. Lack of
knowledge of this condition caused delayed treatment of this
patient. We report here a case of a ganglion of the proximal
interphalangeal joint in a 43 year old Malay lady who was
initially misdiagnosed.
Key words: ganglion, proximal interphalangeal joint,
synovial cyst, swelling
J.Orthopaedics
2006;3(4)e23
Introduction:
Ganglions are the most common soft tissue tumour of the hand.
They are most prevalent in women and generally occur between the
2nd and 4th decades of life 2. Ganglions of the wrist are easily
recognized whereas ganglions of uncommon joints such as the
proximal interphalangeal joint are easily missed as they are
rare.
Case Report
A forty-three year old Malay lady presented to the
Orthopaedic clinic with a one month history of pain and
swelling over the dorsal aspect of the proximal interphalangeal
joint (PIPJ) of the right middle finger following a trivial
injury to her finger. The swelling had progressively increased
in size after the injury and she was unable to flex the finger
fully, however extension of the finger was unaffected.
An X-ray did not reveal any abnormalities and she was
diagnosed to have ligament strain. She was treated
conservatively with analgesics, but as her problem persisted,
she continued to seek other medical opinions before presenting
to the Hand Clinic a year later with the same complaint.
Physical examination
There was minimal swelling over the proximal interphalangeal
joint, and on palpation of this area, there was tenderness over
the ulna aspect of the right middle finger. She was unable to
flex the effected finger fully. There was no weakness of the
fingers nor was there any loss of sensation.
Radiographic findings.
X-Rays were unremarkable.
Diagnosis
Pre-operatively a diagnosis of glomus tumour of the right
middle finger was made. The differential diagnosis considered
were ligament sprain, proximal interphalangeal joint (PIPJ)
synovial cyst and thrombosis of the palmar digital vein.
Treatment
Excision biopsy was carried out on the right middle finger.
An incision was made along the medial side of the right PIPJ of
the right middle finger. A mass measuring 0.1cm X 0.3cm which
was bluish black in color was found adherent to the surface of
the bone. The mass was removed completely, haemostasis was
secured and the wound was closed using Ethilon 6/0 sutures. Post
operatively, the patient was treated with a one week course of
antibiotics (Cloxacillin 500mg QID) and analgesics as needed.
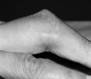
Figure 1 Swelling over ulna
aspect of Right middle finger
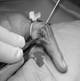
Figure 2 Ganglion arising from PIP joint of Right
middle finger
Discussion :
Ganglions of the proximal interphalangeal joints are
uncommon2,3. Although trauma has been postulated as an inciting
factor, the cause of the ganglions is actually unknown.3. Cheng
et al3 reported 4 patients with this condition who were more
than 65 years of age. Three of these patients were treated by
aspiration and one was surgically treated. Busch et al2 reported
six similar cases, all of whom were surgically treated. Our
patient was only 43 years old. She was treated surgically and
her symptoms resolved after excision of the ganglion with no
recurrence to date.
Ganglions of the PIPJ usually arise from the joint capsule
between the lateral band and the central slip and communicate
with the joint by means of a stalk2. The lesion usually presents
on the ulnar aspect of the extensor mechanism2, and this was
also seen in our patient. Though small, they may interfere with
joint motion. Treatment options of this condition include
observation, aspiration and surgical excision1. In most cases,
observation is acceptable. Indications for more aggressive
treatment include pain, interference with activity, nerve
compression and imminent ulceration. The recurrence rate after
aspiration is 50% for cysts in most locations, whereas
recurrence after surgical excision is only 5% if the stalk of
the cyst along with the small portion of the capsule is
removed1.
Our patient was treated surgically as preoperatively the
lesion was rather small and the diagnosis was not clear;
furthermore as the margins of the swelling were not well defined
aspiration of the lesion was not attempted. The surgical outcome
was satisfactory.
The awareness of this rare condition will be helpful in
making an early and accurate diagnosis.
Reference :
-
Thornburg LE (1999). Ganglions of Hand and Wrist. Journal of
American Academy of Orthopaedic Surgery, 7(4): 231-8.
-
Busch CC, Cable BM, Dabezies EJ (2000). Ganglion of the proximal
interphalangeal joint. Orthopaedics 23(8):839-40.
-
Cheng CA, Rockwell WB (1999). Ganglions of the proximal
interphalengeal joint. American Journal of Orthopaedics , 28
(8): 458-60
|




