Abstract
This article reports an unusual case of
agressive behaviour of a giant-cell tumor of the tendon sheath
involving the thumb that was initially diagnosed as a synovial
sarcoma. This clinical form of presentation of GCTTS is
extraordinarily rare and perhaps can support the possibility of
neoplastic origin.
J.Orthopaedics 2006;3(4)e17
Introduction:
Giant-cell tumor of the tendon sheath (GCTTS)
is the second most common tumor of the hand after ganglia 1.
Before 1941 the lesion had been described under a variety of
names, most of which had the suffic oma, implying a neoplasm
2, although the most widely held theory is that the disease is
an inflammatory reaction of the synovium 3. In recent years,
however, the discussion continues since more recent reports,
including research into the D.N.A of the cells 4 and
immunohistochemically study 5 suggests it to be a neoplastic
process.
This article reports an unusual case of
agressive behaviour of a giant-cell tumor of the tendon sheath
involving the thumb that was initially diagnosed as a synovial
sarcoma. This clinical form of presentation of GCTTS is
extraordinarily rare and perhaps can support the possibility of
neoplastic origin.
Case report
A 76-year-old man presented with a
long-standing soft-tissue mass at the volar aspect of his right
proximal phalange of the thumb that had recently become increase
in size. Physical examination revealed a firm, fixed and diffuse
subcutaneous mass, causing limited flexion at the both
metacarpophalangeal and interphalangeal joints, but without loss
of sensibility. There was no significant tenderness, and no
other nodules were identified. A giant-cell tumor of the
profundus flexor tendon sheat was initially suspected and,
following radiography when no abnormalities were seen (Fig. 1A),
a magnetic resonance imaging (MRI) study was obtained for
further evaluation. MRI revealed a diffuse soft-tissue mass
arising from the flexor tendon sheat of the finger with numerous
little zones of low signal intensity by the presence of
hemosiderin, all of then suggestive of
GCTTS (Fig. 1B).
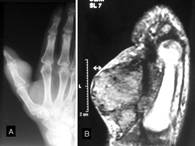 Figure
1: A) Radiograph showing soft-tissue swelling on the volar
surface of the metacarpal bone of the thumb. B) MRI shows
hypointense lesion in the volar aspect of the proximal phalange
of the thumb, attaching to the flexor tendon.
Laboratory data showed no abnormalities.
However, in the interval between the first examination and
surgery (two weeks) the patient returned to the hospital due to
the fast increase of the mass with ulceration of the same over
the skin (Fig. 2). Figure 2: Clinical
picture of the mass. A) Frontal view. B)
Lateral view. Observe the ulceration of the
skin and Figure
1: A) Radiograph showing soft-tissue swelling on the volar
surface of the metacarpal bone of the thumb. B) MRI shows
hypointense lesion in the volar aspect of the proximal phalange
of the thumb, attaching to the flexor tendon.
Laboratory data showed no abnormalities.
However, in the interval between the first examination and
surgery (two weeks) the patient returned to the hospital due to
the fast increase of the mass with ulceration of the same over
the skin (Fig. 2). Figure 2: Clinical
picture of the mass. A) Frontal view. B)
Lateral view. Observe the ulceration of the
skin and 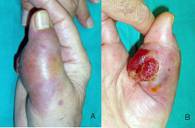 the
protrusion of the
mass, resembling a malignant tumour. the
protrusion of the
mass, resembling a malignant tumour.
Due to the aggressive evolution of the mass
and the possibility of being in the presence of synovial
sarcoma, a both incisional and tru-cut biopsies were performed.
However, histologic examination of the biopsy confirmed the
presence of a GCTTS without evidence of malignancy. The patient
then underwent resection of this mass through a volar zig-zag
approach. Upon dissection through the subcutaneous layer, an
infiltrative mass of brownish-yellow tissue was noted around and
firmly fixed of the flexor sheat but without connection to the
metacarpophalangeal and/or interphalangeal joints and without
any osseous involvement of proximal phalange. After the
dissection and meticulous liberation of the collateral nerves,
the mass was resected until no further tissue was visualized.
Due to the non-vascularized skin flaps, the surgical wound it
itself open. Later and after the clinical follow-up showed a
correct granulation tissue without recurrence of the mass, a
free skin graft of the palmar wrist fold was performed. Six
months later, the patient recovered with complete relief of
symptoms and without evidence of recurrent disease or regrowth
of the residual lesion investigated by MR imaging.
Discussion :
GCTTS is usually a firm, nodular,
well-defined tumour-like mass occurring commonly on the palmar
aspect of the fingers and hand 6. The diagnosis of these lesions
should be include physical examination and radiological study.
GCTTS commonly manifest as a solitary, painless, palpable mass
adherent to the extensor or flexor surface of tendons with a
history of size progression. In general, palpation tenderness or
pain with movement of the joint are infrequent symptoms.
Radiographs show a slightly opaque soft tissue mass, although in
some cases were associated with erosions of the adjacent bones
7,8. These erosions have well-defined sclerotic margins and are
a sign not of malignancy but of direct extension and pressure
effect. Other imaging studies include RMI and sonography. On MRI
the lesions are isointense to muscle on T1-weighted imaging and
hyperintense to the very low signal seen with ganglion cyst. In
some cases they may be slightly hyperintense to muscle because
of the deposition of hemosiderin, which also may bloombing on
gradient echo imaging, as occurred in our case. On T2-weighted
imaging the lesions may be low, intermediate, or high signal,
similar to pigmented villonodular synovitis 9. With respect to
sonographic findings, GCTTS of the hand typically appear as
solid, homogeneous hypoechoic masses with detectable internal
vascularity that are associated with the flexor tendons of the
fingers 10. Finally, when the diagnosis is controversial, fine
needle aspiration cytology o tru-cut biopsies have been found to
correlate well with the final diagnosis 11,12.
When the clinical and radiological
diagnosis was stablished, the treatment of choice is the
complete excision. However it is important to distinguish
between focal and diffuse forms of GCTTS, because both forms are
different rates of recurrence. In this sense and according to
Al-Qattan 1, these lesions were classified into two main types,
depending on whether the entire tumour was, or was not,
surrounded by one pseudocapsule as assessed by the surgeon
during surgery. In Type I the entire tumour is surrounded by one
pseudo-capsule and in consequence easily to perform a complete
excision without recurrences, while in Type II the entire tumour
is not surrounded by one pseudo-capsule and for this reason,
more difficult to perform a complete excision and, and
consequently with a high rate of recurrence 1. In addition, each
type was then sub-classified according to the thickness of the
capsule, lobulation of the tumour, the presence of satellite
lesions, and the diffuse or multicentric nature of the tumour;
these factors were also assessed by the surgeon (Table I).
I. The entire tumour is surrounded by one
pseudo-capsule
- Single nodule with a thick whitish
capsule.
- Single
nodule with a thin capsule.
- Multi-lobulated lesion surrounded by a
common pseudo-capsule.
II. The entire tumor is not surrounded by
one pseudo-capsule
- One main nodule (with a pseudo-capsule)
accompanied by separate satellite lesions within the same
anatomical area.
- Diffuse type with multiple
granular-like lesions with no pseudo-capsule.
- Multicentric type with separate
discrete lesions in the same digit.
Table I: Classification of the giant-cell
tumours of tendon sheat (Al-Qattan, 2001).
In our patient, the tumour was
classified as a Type II b, that is, a diffuse tumour type with
multiple granular-like lesions with no pseudo-capsule. This type
of tumour variant presents a high rate of recurrence after
excision 1. In this context, some authors have noted a higher
recurrence rate for tumours with increased cellularity and
mitotic activity on histological examination, although we could
not find a correlation between these histological features and
recurrence 13,14,15. Recent research shown that giant cell
tumours which are nm 23 negative are more aggressive and are
associated with a high recurrence rate 4. Others significant
risk factors for recurrence included presence of adjacent
degenerative joint disease, location at the distal
interphalangeal joint of the finger or interphalangeal joint of
the thumb, although the most important factor for recurrence was
the poor surgical technique/incomplete excision of the lesion
1,16,17,18. In these cases in which complete excision may not be
possible, radiotherapy may have a role as a prophylaxis against
recurrence 17. However, in our case no radiotherapy was employed
due to presence of skin graft and the probable possibility of
necrosis.
Regarding the underlying nature of this
lesion, specifically whether it is neoplastic or nonneoplastic
process, more controversy exist. Since the first description by
Chassaignac in1852 , which he called cancer of the tendon sheat
19, for many years any tumor containing giant cells was
considered to be a sarcoma 20. It was not even 1941 in which
Jaffe and coworkers 3 suggested that fibrous xanthoma of
synovium and pigmented villonodular synovitis are closely
related conditions which are not true neoplasms, but reactions
to injury. Since then, many authors indicated that the GCTTS is
a nonneoplastic proliferation, if one accepts that a population
of cells forming a tumorous mass must show clonality to be
classified as a neoplasm 21, while others supports a neoplastic
origin 22,23. In general, the natural course of the tumor is
bening 24,25 although in our case, the aggressive behaviour
lesion it could be labeled as neoplastic.
Reference :
-
Al-Qattan MM. Giant cell tumours of tendon
sheat: classification and recurrence rate. J hand Surg 2001; 26
B: 72-5.
-
Flandry F, Hughston J. Current concepts
review: pigmented villonodular synovitis. J Bone Joint Surg
1987; 69 A: 942-9.
-
Jaffe HL, Lichtenstein L, Sutro CJ. Pigmented
Villonodular Synovitis, Bursitis, and Tenosynovitis.
A Discussion of the Synovial and Bursal
Equivalents of the Tenosynovial Lesion Commonly Denoted as
Xantoma, Xanthogranuloma, Giant Cell Tumor or Myeloplaxoma of
the Tendon Sheat, with some Consideration of This Tendon Sheat
Lesion Itsel. Arch Pathol 1941; 31: 731-65.
-
Abdul-Karim FW, El-Naggar AK, Joyce MJ,
Makkley JT, Carter JR. Diffusse and localized tenosynovial giant
cell tumor and pigmented villonodular synovitis: a
clinicopathological and flow cytometric DNA analysis. Human
Pathology 1992; 23: 729-35
-
.Ferrer J, Namiq A, Carda C, López-Gines C,
Tawfik O, Llombart-Bosch A. Diffuse type of giant-cell tumor of
tendon sheat: an ultrastuctural study of two cases with
cytogenetic support. Ultrastruct Pathol 2002; 26: 15-21.
-
Jones FE, Soule EH, Coventry MB. Fibrous
Santhoma of Synovium (Gian-Cell Tumor of Tendon Sheat, Pigmented
Nodular Synovitis). A Study of One Hundred and Eighteen Cases. J
Bone Joint Surg 1969; 51 A: 76-86.
-
Uriburu IJF, Levy VD. Intraosseous growth of
giant cell tumors of the tendon sheat (localized nodular
tenosynovitis) of the digits: report of 15 cases. J Hand Surg
1998; 23 A: 732-6.
-
Karasick D, Karasick S. Giant cell tumor of
tendon sheath: spectrum of radiologic findings. Skeletal Radiol.
1992;21:219-224.
-
Jelinek JS, Kransdorf MJ, Shmookler BM,
Aboulafia AA, Malawer MM. Giant cell tumor of the tendon sheat:
MR findings in nine cases. Am J Roentgenol 1994; 162: 919-22.
-
Middleton WD, Patel V, Teefey SA, Boyer MI.
Giant cell tumors of the tendon sheat: analysis of sonographic
findings. AJR 2004; 183: 337-9.
-
Agarwal PK, Gupta M, Srivastava A, Agarwal S.
Cytomorphology of giant cell tumor of tendon sheat. Acta
Cytologica 1997; 41: 587-9.
-
Choudhury , Jain R, Nangia A, Logani KB.
Localized tenosynovial giant cell tumor of tendon sheat. Acta
Cytologica 2000; 44: 463-6.
-
Rodrigues C, desai S, Chinoy R. Giant cell
tumor of the tendon sheat: a retrospective study of 28 cases. J
Surg Oncol 1998; 68: 100-3.
-
Byers PD, Cotton RE, deacon OW. The diagnosis
and treatment of pigmented villonodular synovitis. J Bone Joint
Surg 1968; 50 B: 290-305.
-
Rao As, Vigorita Vj. Pigmented villonodular
synovitis (giant cell tumor of the tendon sheat and synovial
membrane). J Bone Joint Surg 1984; 66 A: 76-94.
-
Grover R, Grobbelaar AO, Richman PI, Smith PJ.
Measurement of invasive potential
provides an accurate prognostic marker for giant cell tumour of
tendon sheat. J Hand Surg 1998; 23 B: 728-31.
-
Kotwal PP, Gupta V, Malhotra R. Giant-cell
tumour of the tendon sheat. Is radiotherapy indicated to prevent
recurrence after surgery ?. J Bone Joint Surg 2000; 82 B: 571-3.
-
Reilly KE, Stern PJ, Dale A. Recurrent giant
cell tumors of the tendon sheat. J Hand Surg 1999; 24 A:
1298-302.
-
Chaissagnac M. Cancer de la gaine des tendons.
Gaz hosp civ milit 1852 ; 47 : 185-6.
-
Heurtaux MA. Myélome des gaines tendineuses.
Arch Gen Med 1891 ; 167 : 40-54.
-
Vogrincic GS, OConnell JX, Gilks CB. Giant cell
tumor of tendon sheat is a polyclonal cellular proliferation.
Hum Pathol 1997; 28: 815-9.
-
Nielsen AL, Kiaer T. Malignant cell tumor of
synovium and locally destructive pigmented villonodular
synovitis: ultrastructural and immunohistochemical study and
review of the literature. Hum Pathol 1989; 20: 765-71.
-
Walsh EF, Mechrefe A, Akelman E, Schiller AL.
Giant cell tumor of tendon sheat. Am J Orthop 2005; 34: 116-21.
-
Uriburu IJF, Levy VD. Intra-osseous growth of
giant cell tumors of the tendon sheat (localized modular
tenosynovitis) of the digits: report of 15 cases. J Hand Surg
1998; 23 A: 732-6.
-
shijima M, Hashimoto H, Tsuneyoshi M, Enjoji
M. Giant cell tumour of the tendon sheat (nodular tenosynovitis):
a study of 207 cases to compare the large joint group with the
common digit group. Cancer 1986; 57: 875-84.
|




