|
*A. Elmrini, A. Daoudi,
O. Agoumi, F. Boutayeb, M. Mahfoud, A. Elbardouni, M. Elyaacoubi.
*Department of orthopaedics, UH Hassan II
Fez, UH Avicenne Rabat; Morocco.
Address for Correspondence
Dr. A. ELMRINI
Department of Orthopedic and Traumatic Surgery
Al Ghassani Hospital, University Hospital Hassan II, Fez 30000.
Morocco
Tel: 00 212 61 107 741, Fax: 00 212 55 619 321
E-mail: traumajid@yahoo.fr
|
|
J.Orthopaedics 2006;3(3)e17
Introduction:
Fracture
dislocations of the femoral head remain extremely rare fracture
of the hip. The isolated fracture is not reported in the
literature. Therefore, we report in this manuscript unusual
lesion in the form of a shifting of the femoral head, this has
had favorable evolvement after opened reduction and internal
fixation.
Case
Report
Our patient is a male of 38
years old without any particular history of pathology. He was a
victim of a traffic accident with fall from his motorcycle. He
was received on side and on the right knee.
This caused a traumatism of the
right hip. At the admittance in the hospital, the patient
suffered from severe pains and a functional disability of the
right lower member. The clinical examination did not reveal
deformation, but showed existing pain at the mobilization of the
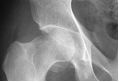
hip. There were no other associated lesions. The X-rays of the
right hip objectified a fracture of the femoral head with an
osseous defect of the superior pole, and two osseous fragments
falling behind; the joint was not dislocated (Figure 1). The
CT-scan showed a fragmentation of
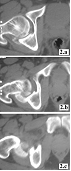
the femoral head with multiple
fragments, but remaining in the cotyle which was intact (Figure
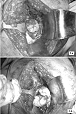
2). The surgical access was posterior and the exploration
discovered a cartilage shift in 3 big cuttings (Figure 3.a).
The reduction has required the dislocation of the head
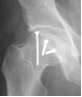
(Figure 3.b) with buried screwing. The post-surgery control
showed a good reduction of the fracture with a spherical head
(Figure 4). After a discharge of 6 weeks, the support was
achievable without pain. The result is good after 14 months. The
hip is pain free, stable with good normal motion. There is no
necrosis of the femoral head.
Discussion :
The femoral head fractures are
very rare, they are always associated to a dislocation of the
hip, and the posterior variety remains the most frequent. The
consequences of these hurts are very grave. The etiology is
dominated by the accidents of the public road [1].
The dislocation factors are
dismembered according to several classifications, according to
the displacement [2]. The isolated fracture of the femoral head
is not reported in the adopted classifications. Pipkin
established in 1957 a classification, which states 4 stages,
which are all associated to posterior dislocation of the hip.
The type I a dislocation of the hip associated to a fracture
under fovea; in the stage II, the fracture catches the fovea.
The stage III is a lesion of type I or II associated to a
fracture of the femoral colles; while the stage IV encloses a
fracture of the acetabulum [3].
The classification of Brumback
is more exhaustive [4]; and described 5 types. The type I
represents a posterior dislocation with inferomedial fracture;
in the type II, the fracture is superomedial ; the type III
associates a dislocation of the hip without clarifying its
direction together with a fracture of the femoral neck; Type IV
contains the previous dislocations associated to the cephalic
fractures. The type V described fractures with central
dislocation. This classification can contain the "shifting" of
the femoral head without dislocation in type II.
The face X-ray of the pond
allows revealing any asymmetry even small, which must make be
suspect. The centered X-ray studies more precisely the reasons
of both, hillsides of the joint in search of past unnoticed
fractures [5].
The CT-scan operated in thin
slices, clarifies the site of the lesion, or a confinement. This
study is essential in case of instability, an asymmetry of
interlines and the fracture of the head or the cotyle; this to
define better the lesions [6-8]. The arthrography, the arthro-CT
[9] or the magnetic resonance imaging (MRI) were evoked.
The conservative treatment is
the rule in case of the types 1 and 2 [10]; the surgical
reduction would become necessary. The access procedure depends
at first on the variety of the dislocation and on the movement
of fragments. The Kocher Langenbeck access can be used for
fractures associated to the posterior wall of the cotyle. Some
authors use a trochanterotomy for improving the visibility and
facilitate the osteosynthesis [11, 12]. The approach of Smith
Peterson is used in case of previous dislocation [2, 13]. We
used at first posterior approach guided by the movement of
fragments. The osteosynthesis require a buried screwing using a
metal or bio-resorbed material [14, 15]. The small fragments can
be resected [16, 17].
The complications are frequent.
Necrosis risks of the femoral head are situated between 0 and 24
%. The degenerative posttraumatic osteoarthritis is between 0
and 72 %; the nervous lesions are between 7 and 27 % and
heterotopic ossifications are between 2 and 54 % [12].
The isolated fractures communitive of the femoral head, are
recognized as cartilaginous shifting of difficult treatment. The
posterior approach leads good exposition for internal fixation
without avascular necrosis.
Reference :
- Durabkasa O, kan N, Canbora K, Gorgec M. Factors affecting
the results of treatment in traumatic dislocation of the hip.
Acta Othop Traumatol Turc. 2005; 39 (52): 133-41.
- Bauer GJ, Sarkar MR. Injury classification and
surgicalapproach in hip dislocations and fractures. Orthopade
1997; 26(4): 304-16.
- Pipkin G. Treatment of grade IV fracture dislocation of
the hip. J Bone JOIN Surg Am 1957; 39-A (5):1027-42.
- Brumback RJ, Kenzora JE, Levitt LE, Burgess AR, Poka A.
Fractures of the femoral head. In: The Hip Society, editor.
Proceeding of the hip Society, 1986. St. Louis: Mosby; 1987;
p.181-206.
- Sontich JK, Cannada LK. Femoral head avulsion fracture
with malunion to the acétabulum: a case report. J Orthop
Trauma.2002; 16(1): 49-51.
- Ordway B, Xeller CF. Transverse computerized axial
tomography of patients with posterior dislocation of the hip.
J Trauma 1984; 24: 76-79.
- Hougaard K, Thomsen PB Coxarthrosis following traumatic
posterior dislocation of the hip. J Bone Joint Surg 1987;
69-A: 679-683.
- Yang RS, TsuangYH, Hang YS, Liu TK Traumatic dislocation
of the hip. Clin Orthop 1991; 265: 218-227
- Canale ST, Manugian AH. Irreducible traumatic dislocations
of the hip. J Bone Joint Surg 1979 ; 61-A : 7-14
- Matejba J, Koudela K. Bilateral fractures of the femoral
head 5 Pipkin I and Pipkin II). Acta Chir Orthop Traumatol
Cech.2002; 69(6): 369-71.
- Ganz R, Gill TJ, Gautier E, Ganz K, Krugel N, Berlemann
U. Surgical dislocation of the adult hip a technique with full
access to the femoral head and acétabulum without the risk of
avascular necrosis. J Bone Joint Surg Br 2001 ; 83(8):1119-24
- Kloen P, Sienbenrock KA, Raymakers ELFB, Marti RK, Ganz R.
Femoral head fractures revisited. Eur J Trauma 2002; 28:
221-33.
- Shonweiss T, Wagner S, Mayr E, Ruter A. Klinik fur Unfall
Und Wiederherstellungschirurgie, Zenttralklinikum Augsburg.
Unfallchirurg. 1999; 102 (10):776-83.
- Hermus JPS, Laan CA, Hogervorvorst M, Rhemrev JS. Fixation
of Pipkin fracture with bio-absorbable screws case report and
review of the literature. Injury 2005 (36);458-461
- Prokop A, Helling HJ, Hahn U, Udomkaewknjana C, Rehm KE.
Biodegradable implants for Pipkin fractures. Clin Orthop Relat
Res. 2005; (432):226-33.
- Holmes WJ, Solberg B, Bay BK, Laubach JE, Olsen SA.
Biomechanical consequences of excision of displaced Pipkin
femoral head fractures. OTA 1999 Oct; Session VIII.
- Siebenrock KA, Gautier E, Woo AK, Ganz R. Surgical
dislocation of the femoral head for joint debridement and
accurate reduction of fractures of the acétabulum. J Orthop
Trauma 2002; 16(8): 543-52.
|






